Ozone Therapy for Stroke, Traumatic Brain Injuries, and Other Brain Damages
At a Glance:
- Ozone therapy can help with neurorecovery by rebalancing oxidative stress and inflammation, increasing BDNF, protecting mitochondrial function, and supporting the gut barrier.
- Based on the limited clinical evidence available, systemic ozone treatments like autohemotherapy and rectal insufflation led to meaningful reductions in symptoms and improvements in neurologic markers. These protocols involve initially frequent treatments, followed by regular use as the patients recover.
- Ozone rectal insufflation in particular may assist with brain recovery through helping the gut barrier and improving the gut flora.
- Ozone therapy is not a replacement for conventional treatments and rehabilitation, but may be added on as a supportive treatment in consultation with your care team.
Ozone therapy also has brain-regenerative benefits, as several clinical trials have indicated positive outcomes in stroke and traumatic brain injury patients. In this article, we’ll cover why ozone therapy may help for these conditions along with the existing clinical evidence.
Amber’s Story:
I had a stroke 16 months ago. The massive stroke, giant clot, went into the Broca’s area, which means all my vocabulary, all the English language, reading, writing, and all my math problems were what I really had a hard time with. My entire left side of my body was paralyzed. I was doing ozone treatments with the UBI and it’s made a huge difference. Within about 2 months we went to a clinic and did a SPECT scan. They said my brain looked like I had a stroke 2 years ago, not 2 months ago. They wanted me to come back in 2 years to do a study on me, since my vocabulary came back after I did ozone.
Why Might Ozone Therapy Help With Brain Damages?
Stroke, traumatic brain injury (TBI), and other forms of acquired brain damage share a common biological theme:
- Ischemia, or damage from temporary lack of oxygen
- Oxidative stress
- Inflammation
- Mitochondrial dysfunction
Although the initiating event may differ, i.e., blood vessel blocks in stroke and mechanical trauma in TBI, the downstream cascade is remarkably similar.
Neurons become metabolically unstable, inflammatory signaling escalates, blood–brain barrier (BBB) integrity is disrupted. Glutamate and oxidative stress increase, which can snowball into secondary damage long after the initial event.
Ozone therapy modifies many of these processes simultaneously, both in the short and long term, making it a helpful adjunctive modality for recovery from stroke and TBI.
Timing Matters
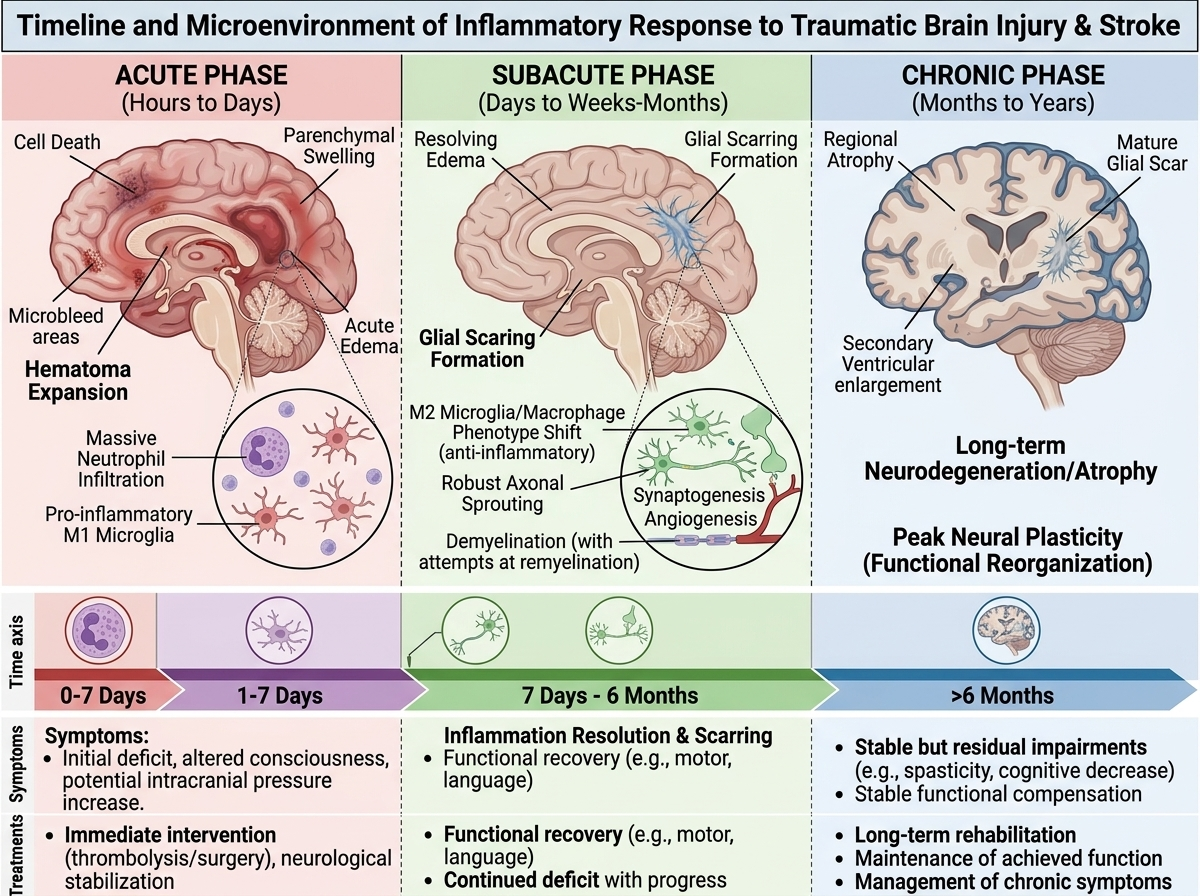
The inflammatory response after brain injury follows a predictable progression:
- Acute phase: Intense oxidative burst and cytokine release.
- Subacute phase: Ongoing microglial activation, mitochondrial dysfunction, and reduced brain blood flow can snowball into secondary damage.
- Chronic phase: Low-grade inflammation and impaired repair.
Interventions like ozone that modulate oxidative stress may be most relevant in the subacute and early recovery phases, when limiting secondary injury can meaningfully influence outcomes.
Ozone is not a replacement for acute neurological care or even rehabilitation. Rather, its potential role would be as an adjunctive strategy aimed at reducing secondary injury and supporting recovery.
Past the acute phase, ozone therapy can support recovery through modulating inflammatory and oxidative response.
Here are possible ways that it may help.
Nrf2 Activation Improves BDNF
Ozone therapy produces secondary byproducts that cross into the blood–brain barrier and can activate Nrf2.
BDNF is a neurotrophic protein, which works as a fertilizer for your brain. It supports neuronal survival, synaptic plasticity, axon regeneration, learning, memory, and post-injury recovery [1]. Not surprisingly, BDNF levels are crucial for the recovery from any brain damage.
Nrf2 (nuclear factor erythroid 2–related factor 2) is a cellular manager that mainly manages antioxidant genes, such as glutathione production and superoxide dismutase-encoding genes [2]. In addition, Nrf2 also manages the production of BDNF.
Small amounts of oxidative stress from hormetic treatments like ozone therapy activate both Nrf2 and BDNF, similar to the way exercise or sauna use do.
In stroke and TBI, oxidative stress overwhelms endogenous antioxidant systems. Neurons are particularly vulnerable due to their high oxygen demand and lipid-rich membranes.
Activation of Nrf2 shifts the intracellular environment from pro-oxidative to protective, reducing secondary injury cascades. Medical ozone, through transient redox signaling (H₂O₂ and lipid mediators such as 4-HNE), can activate the Nrf2 pathway systemically and in the brain [3].
This hormetic activation increases endogenous antioxidant capacity rather than acting as a direct antioxidant itself.
After stroke or traumatic brain injury, BDNF levels often decline in the acute phase, contributing to impaired neuroplasticity and reduced functional recovery [4].
Emerging research suggests that Nrf2 activation can increase BDNF [5] through the following possible mechanisms:
- Reduction in oxidative stress improves CREB signaling upstream of BDNF, thus improving BDNF production [6].
- Nrf2-mediated antioxidant protection stabilizes mitochondrial function, preserving neuronal energy necessary for neurotrophin synthesis [7].
- HO-1 and related Nrf2-managed genes modulate neuroinflammation, creating an environment that makes it easier for BDNF to do its job [8].
In animal models of cerebral ischemia, Nrf2 activation with drugs improved neurological outcomes and increased BDNF expression in peri-infarct tissue [9].
Similarly, redox-modulating interventions that enhance endogenous antioxidant capacity often correlate with improved neuroplastic signaling.
Why Nrf2 and BDNF Matter in Brain Injury
To recover well from these types of damage, your brain needs to limit secondary damage and also rewire or repair the injury. High BDNF is generally correlated with positive outcomes, as it helps with [10]:
- Cortical reorganization after stroke
- Synaptic remodeling after TBI
- Long-term cognitive recovery
- Reducing the risk or severity of depression, which can impact the overall outcomes
If ozone therapy activates Nrf2 in a controlled, hormetic manner, it may indirectly enhance BDNF signaling through improved cellular redox balance.
Redox Preconditioning and Neuroplasticity
Oxidative preconditioning is well established in neuroscience. Mild, controlled oxidative stimuli can upregulate protective genes and improve resilience to future insults.
Exercise is a well-known example of this phenomenon, as it robustly increases BDNF [11].
Ozone-induced Nrf2 activation operates through a similar hormetic principle: enhancing endogenous defense systems and potentially supporting neuroplastic processes during recovery [12].
While direct clinical trials examining ozone therapy, Nrf2 activation, and BDNF in stroke or TBI populations are limited, the biological plausibility is strong:
- Stroke and TBI involve oxidative overload.
- Nrf2 protects neurons in ischemic models.
- Nrf2 signaling supports BDNF expression.
- Ozone therapy activates Nrf2 through redox signaling.
This intersection suggests how ozone therapy could support brain repair processes, particularly in subacute or recovery phases.
Ozone Therapy Helps Manage Inflammation and Oxidative Stress
Inflammation and oxidative stress are central drivers of ongoing neural damage. You get the initial damage where the body responds with inflammation and oxidative stress. Subsequently, these can snowball into a secondary injury cascade that can persist for days to weeks, fueled by [13,14]:
- Excess reactive oxygen species (ROS)
- Lipid peroxidation
- Microglial activation
- Cytokine release (IL-1β, TNF-α, IL-6)
- Mitochondrial dysfunction
- Excitotoxic signaling
Unchecked, this environment promotes neuronal cell death (apoptosis), impairs synaptic recovery, and worsens long-term neurological outcomes.
Ozone therapy helps by supporting the body to better modulate the inflammation and oxidative stress so the brain can heal.
Redox Modulation
Ozone therapy provides a small dose of oxidative stress that creates lipid oxidation byproducts and hydrogen peroxide. These molecules trigger antioxidant cellular pathways like Nrf2, increasing glutathione and antioxidant enzymes [15].
Rather than eliminating reactive oxygen species outright, ozone therapy recalibrates oxidative signaling toward a more balanced state.
This is particularly relevant in brain injury, where excessive ROS production overwhelms your body’s antioxidant capacity.
By strengthening intrinsic defense systems, ozone therapy may help limit ongoing lipid peroxidation and mitochondrial instability in the subacute phase of injury.
Inflammation Regulation
Following stroke or TBI, activated microglia and peripheral immune cells release pro-inflammatory cytokines that can create more tissue damage [16,17].
Elevated IL-1β, IL-6, and TNF-α are commonly observed and correlate with worse outcomes [18].
Ozone therapy research, both clinical and preclinical, in other inflammatory conditions has demonstrated [19]:
- Reduction in excessive pro-inflammatory cytokine production
- Modulation of NF-κB signaling
- Improved balance between pro- and anti-inflammatory mediators
Importantly, ozone’s immunomodulatory effects appear to be regulatory rather than suppressive. Unlike corticosteroids, ozone therapy does not suppress immune responses but rather restores balance in the whole body. This systemic inflammation management may indirectly support central nervous system recovery.
Lipid Peroxidation Control and Membrane Protection
Neuronal membranes are rich in polyunsaturated fatty acids and are susceptible to oxidative damage [20].
Lipid peroxidation products such as malondialdehyde (MDA) and 4-HNE increase after stroke and TBI, contributing to membrane instability and mitochondrial dysfunction [21].
Ozone therapy can deliver benefits by creating some of these byproducts in the blood, but at a much smaller doses, which stimulate physiologic responses resulting in [22]:
- Decreased baseline levels of lipid peroxidation markers
- Improved redox enzyme activity
- Enhanced cellular resilience to oxidative challenges
This adaptive response may reduce susceptibility to secondary oxidative waves that occur after the initial injury.
Microglial Balance and Recovery
Microglial cells are housekeeping and immune cells in your brain. They typically take care of your neurons, cleaning up debris, pruning unnecessary synapses, and maintaining balance.
When there is brain injury, microglial cells are activated into a pro-inflammatory form (M1-like) before turning into a pro-repair state.
Sometimes, when you have excessive inflammation and oxidative stress, the microglial cells can get stuck in M1 form.
In the test tube, low-dose ozone can help modulate microglial status and function, minimizing the microglia’s chronic neuroinflammatory state [23].
Brain injury is not an isolated event confined to neural tissue. Immune activation outside the brain, such as in the blood and gut, can also influence microglial status, along with brain inflammation and healing.
By activating Nrf2, managing oxidative stress, modulating whole-body inflammation,and improving microcirculation, systemic ozone treatments can help with stroke or TBI recovery by modulating microglial activation [24].
Ozone Therapy Supports and Preserves Mitochondrial Function
Mitochondrial dysfunction is a defining feature of both ischemic stroke and traumatic brain injury [25,26].
Neurons are among the most energy-demanding cells in the body. Brain injuries typically disrupt brain blood flow, sometimes to less than 20% of normal, cutting off crucial nutrients and oxygen [27].
When cerebral blood flow is interrupted or when mechanical trauma disrupts cellular integrity, mitochondria rapidly lose the ability to maintain energy production, membrane potential and balance, and oxidative signaling [28].
This dysfunction triggers cell death and further oxidative injury. This is called the secondary injury cascade [29].
Because mitochondrial failure and excessive oxidative stress cause further damage, any intervention that improves mitochondrial resilience can theoretically support recovery.
Improvement in Brain Oxygenation
In addition to antioxidant upregulation, ozone therapy improves red blood cell flexibility and 2,3-bisphosphoglycerate (2,3-BPG) levels [30,31]. 2,3-BPG helps red blood cells release more oxygen. This makes oxygen more available to peripheral tissues and the brain.
This helps the oxygen-starved metabolically vulnerable neurons, along with mitochondrial function [32].
Protection Against Mitochondrial Lipid Peroxidation
Mitochondrial membranes contain cardiolipin, a phospholipid highly susceptible to oxidative damage. Cardiolipin peroxidation destabilizes cytochrome c and promotes apoptotic signaling [33].
Repeated low-dose ozone exposure has been associated in experimental models with [34]:
- Decreased baseline lipid peroxidation markers
- Increased antioxidant enzyme capacity
- Reduced susceptibility to oxidative membrane injury
This hormetic adaptation may help preserve mitochondrial structural integrity in the setting of ongoing oxidative stress.
Ozone Rectal Insufflation Supports the Gut Barrier
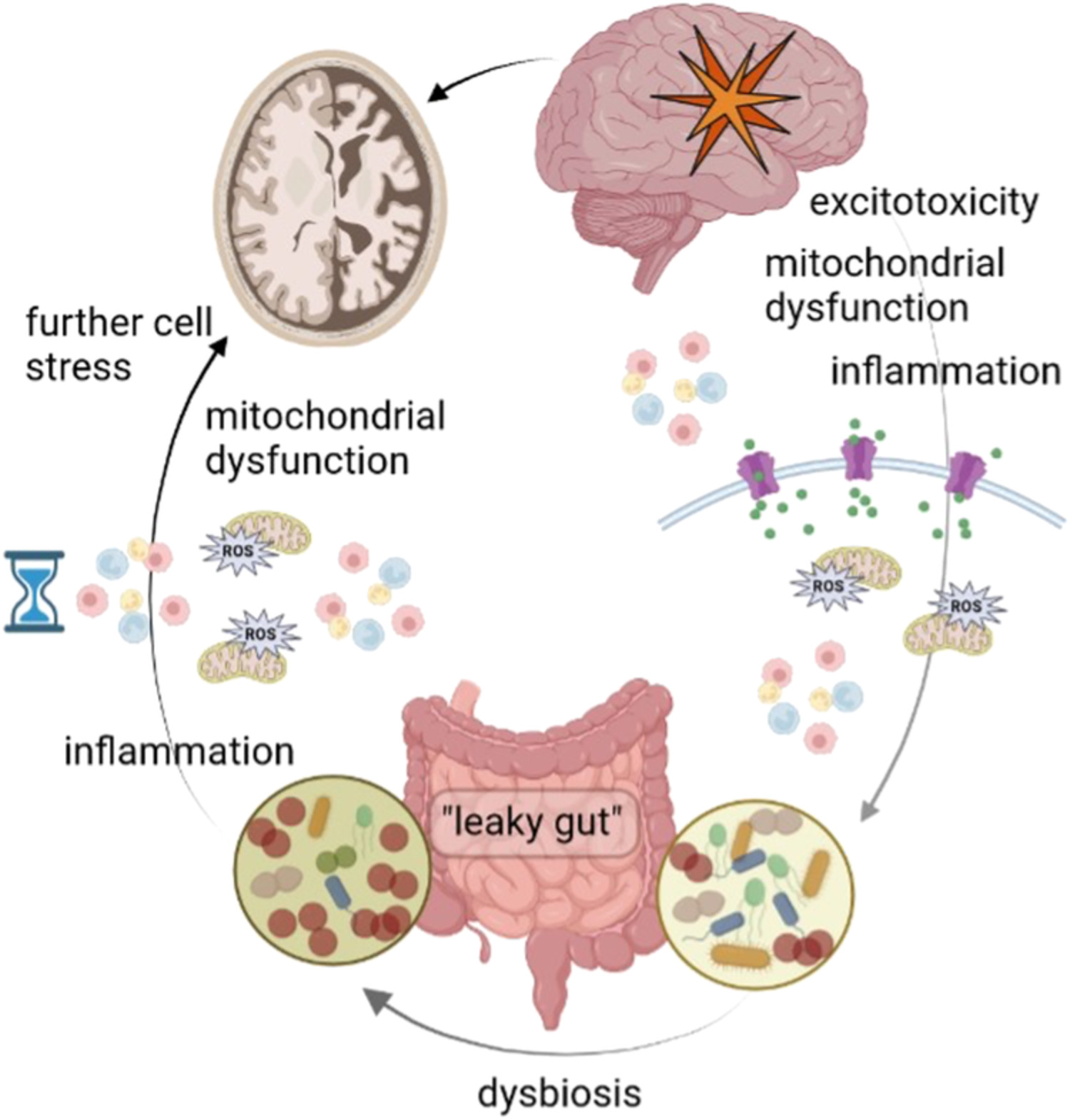
Stroke and traumatic brain injury are increasingly recognized as whole-body inflammatory events, not purely brain injuries. The gut plays a bigger role than most people think.
After acute brain injury, you get intestinal barrier dysfunction (“leaky gut”), dysbiosis, and bacterial translocation. This exposes the gut content and bacterial parts to the gut immune system, increasing systemic inflammation. This whole-body inflammation can further worsen neuroinflammation and recovery trajectories [35,36].
This means poor diet, pre-existing gut issues, or the lack of support for gut barrier repair can contribute to worse outcomes.
Why Gut Support Modalities Are Being Explored in Stroke/TBI Recovery
Because the gut barrier dysfunction can amplify the inflammation, stroke researchers have actively explored whether gut-targeted interventions might influence outcomes.
The American Heart Association review on the microbiota–gut–brain axis in stroke discusses preclinical and emerging translational work involving microbiome manipulation (e.g., antibiotics, probiotics, fecal microbiota transfer) and how gut permeability/translocation is linked with post-stroke inflammation and complications [38].
The takeaway is not that the gut is the sole driver, but that gut homeostasis can strongly influence recovery.
Where Rectal Ozone Insufflation Fits
Although rectal ozone insufflation (RI) is a systemic ozone treatment, it also delivers many gut-specific benefits, including normalizing gut barrier inflammation and improving the gut flora.
A clinical study in ulcerative colitis reported that ozone therapy combined with standard therapy (sulfasalazine delivered via a colon therapy system) was associated with more rapid symptom improvement and better histologic improvement than comparison groups, with no adverse effects reported in that study context [39].
While ulcerative colitis is not stroke/TBI, it suggests that RI can influence intestinal inflammation and mucosal architecture, creating a better environment for healthy flora. Potentially, the small amount of oxidative stress and oxygen can jumpstart the mitochondria and normalize immune responses in the gut barrier.
Also, preclinical work suggests that RI and ozone water enema can improve dysbiosis, potentially by modulating pathways such as SIRT1–Nrf2/HO-1 in mice [40].
Nrf2 signaling helps maintain epithelial resilience and barrier function, in part by supporting antioxidant defenses and tight-junction-related homeostasis under stress [41].
Therefore, it is reasonable to hypothesize that gut-centered ozone delivery could support gut inflammatory balance and barrier resilience, which may indirectly reduce systemic inflammatory load during brain injury recovery.
Clinical and in Vivo Evidence for Ozone Therapy for Recovery from Stroke, TBI, and Other Brain Damage
Stroke
An RCT evaluated the efficacy of ozonated autohemotherapy (O₃-AHT) in 62 patients with acute cerebral infarction [42].
Patients with moderate stroke severity (NIHSS 4–15) were enrolled. The treatments over 5 consecutive days were started within 24 hours of symptom onset after patients were randomized into three groups:
- Standard control group
- Oxygen placebo group
- Ozone therapy group
Ozonated autohemotherapy resulted in:
- 30% decrease in NIHSS scores relative to the control group, indicating meaningful reduction in neurological deficits.
- 25% increase in Barthel index scores, reflecting improved activities of daily living and functional independence.
- 20% improvement in MoCA (Montreal Cognitive Assessment) scores, suggesting measurable cognitive benefit.
- 25% decrease in Neuron-Specific Enolase (NSE) and 30% decrease in S100β protein (p < 0.05), markers for neuronal injury.
- Significantly decreased malondialdehyde (MDA), a marker of lipid peroxidation.
- Increases in glutathione peroxidase (GSH-Px), an antioxidant marker.
- Increased gene expression of Nrf2 (nuclear factor erythroid 2–related factor 2) and HIF-1 (hypoxia-inducible factor 1).
Ozonated autohemotherapy administered early after cerebral infarction was associated with improved neurological scores, reduced neuronal injury biomarkers, and modulation of oxidative stress pathways.
Traumatic Brain Injuries
A clinical study evaluated whether ozone autohemotherapy (OA) could mitigate secondary myocardial injury in 40 patients with acute traumatic brain injury (TBI) [43].
The OA group received ozone autohemotherapy preoperatively and on postoperative days 1 and 2. The control group received autologous blood transfusion without ozone exposure.
Assessments were conducted at baseline (T0) and 7 days post-surgery (T1).
OA treatment resulted in:
- Significantly increased cTnT levels from T0 to T1 in both groups (p < 0.01)
- This indicated that secondary myocardial injury occurred following TBI in all patients.
- Significantly lower NT-proBNP levels at T1 (p = 0.021), suggesting reduced cardiac stress
- Significantly higher left-ventricular ejection-fraction (LVEF) (p = 0.002)
- Significantly higher SOD levels (p = 0.015), indicating enhanced antioxidant capacity
- Significantly shorter ICU length of stay (p = 0.021)
- Significantly reduced total hospitalization time (p = 0.015)
Perioperative ozone autohemotherapy in acute TBI patients was associated with improved cardiac function markers, enhanced antioxidant activity, and shorter hospitalization time.
Larger randomized trials are needed to confirm these results and assess long-term outcomes.
Ischemic Injuries
An animal study investigated whether ozone pretreatment protects against myocardial ischemia/reperfusion injury (MIRI) through inhibition of the NLRP3 inflammasome [44].
Rats received rectal ozone infusion for 5 consecutive days prior to injury induction. Myocardial ischemia was induced via ligation of the left anterior descending (LAD) coronary artery for 30 minutes, followed by 120 minutes of reperfusion.
The NLRP3 inflammasome plays a central role in this inflammatory cascade by activating caspase-1 and promoting secretion of pro-inflammatory cytokines such as IL-1β and IL-18.
Ozone pretreatment resulted in:
- Significantly improved diastolic cardiac function (p < 0.05)
- Significantly reduced myocardial infarct size (p < 0.05)
- Reduced myocardial structural damage on H&E staining
- Significantly reduced molecular markers (p < 0.05), including:
- NLRP3 expression
- ASC (apoptosis-associated speck-like protein)
- Pro-caspase-1
- Active caspase-1
- IL-1β
- IL-18
These findings indicate suppression of inflammasome-mediated pyroptotic signaling leading to improved cardiac function.
Further studies are needed to determine translational relevance to human ischemic disease.
Post-infection Neurologic Symptoms
A case report described the use of oxygen–ozone therapy in a 14-year-old boy with acute meningoencephalitis followed by post-infectious chronic fatigue syndrome (CFS) and a previously treated elite athlete with post-infectious CFS [45].
The 14-year-old presented with:
- Hyperpyrexia (39°C)
- Severe headache, dizziness, and prolonged vomiting
- Elevated CSF protein (129 mg/dL) and serology positive for HSV-1 IgG, EBV IgG (VCA and EBNA), CMV IgG
Although the patient received treatment (IV ceftriaxone for 8 days and IV acyclovir for 12 days) to resolve the fever, all the other symptoms remained. The patient then received rectal ozone insufflation (150 cc at 35 mcg concentration) twice weekly for 4 weeks, then weekly for an additional 4 weeks.
Ozone treatment resulted in:
- Complete remission of weakness symptoms
- Regression of neurologic symptoms and a normal neurological exam
- Improved autoimmune markers (Normalized ENA antibodies; SSA weakly positive but borderline)
Maintenance ozone therapy was continued monthly, then bimonthly.
In the case of the elite athlete, the patient presented with persistent fatigue, anxiety, polymyalgia, and cognitive symptoms, along with a history of toxoplasmosis and mononucleosis. Previous symptomatic therapy (analgesics, anxiolytics) was ineffective.
The patient then received 4 sessions of ozone autohemotherapy (35 mcg per 100 cc blood) followed by 8 rectal ozone insufflations (35 mcg concentration).
Ozone treatment resulted in:
- Remission of weakness and neurological symptoms
- Normalization of lab parameters
- Return to elite physical performance (the patient later won a world championship)
This report described tangible symptomatic improvement in two post-infectious neurological fatigue syndromes following oxygen–ozone therapy. While important, the evidence level is low, and would benefit from clinical trials to confirm efficacy in post-infectious meningoencephalitis or CFS populations.
Conclusion:
Ozone therapy can be a powerful supportive modality for brain recovery, whether it’s after a brain injury, a stroke, toxic exposure, or an infection. However, it doesn’t replace conventional treatments or rehabilitation. Although ozone therapy is very safe, if you decide to add it to your recovery program, it should be started carefully and slowly in consultation with an experienced practitioner.
References:
1 Bathina, S. and Das, U. N. (2015) Brain-derived neurotrophic factor and its clinical implications. Arch. Med. Sci., Termedia Sp. z.o.o. 11, 1164–1178
2 He, F., Ru, X. and Wen, T. (2020) NRF2, a transcription factor for stress response and beyond. Int. J. Mol. Sci., MDPI AG 21, 4777
3 Cisterna, B., Costanzo, M., Nodari, A., Galiè, M., Zanzoni, S., Bernardi, P., et al. (2020) Ozone activates the Nrf2 pathway and improves preservation of explanted adipose tissue in vitro. Antioxidants (Basel), MDPI AG 9, 989
4 Shan, D., Zheng, Y. and Froud, K. (2021) Brain-derived neurotrophic factor as a clinical biomarker in predicting the development of post-stroke depression: A review of evidence. Cureus, Springer Science and Business Media LLC 13, e15662
5 Fath, J., Brouillard, F., Claverie, D., Cabayé, A., Nuss, P., Chwetzoff, S., et al. (2025) BDNF exerts an NRF2-dependent cytoprotective function via a receptor-independent pathway. Cell Rep., Elsevier BV 44, 116587
6 Hayes, J. D., Dayalan Naidu, S. and Dinkova-Kostova, A. T. (2025) Regulating Nrf2 activity: ubiquitin ligases and signaling molecules in redox homeostasis. Trends Biochem. Sci., Elsevier BV 50, 179–205
7 Holmström, K. M., Kostov, R. V. and Dinkova-Kostova, A. T. (2016) The multifaceted role of Nrf2 in mitochondrial function. Curr. Opin. Toxicol., Elsevier BV 1, 80–91
8 O’Rourke, S. A., Shanley, L. C. and Dunne, A. (2024) The Nrf2-HO-1 system and inflammaging. Front. Immunol., Frontiers 15, 1457010
9 Yao, W., Lin, S., Su, J., Cao, Q., Chen, Y., Chen, J., et al. (2021) Activation of BDNF by transcription factor Nrf2 contributes to antidepressant-like actions in rodents. Transl. Psychiatry, Springer Science and Business Media LLC 11, 140
10 Failla, M. D., Juengst, S. B., Arenth, P. M. and Wagner, A. K. (2016) Preliminary associations between brain-derived neurotrophic factor, memory impairment, functional cognition, and depressive symptoms following severe TBI. Neurorehabil. Neural Repair, SAGE Publications 30, 419–430
11 Szuhany, K. L., Bugatti, M. and Otto, M. W. (2015) A meta-analytic review of the effects of exercise on brain-derived neurotrophic factor. J. Psychiatr. Res., Elsevier BV 60, 56–64
12 León, O. S., Menéndez, S., Merino, N., Castillo, R., Sam, S., Pérez, L., et al. (1998) Ozone oxidative preconditioning: a protection against cellular damage by free radicals. Mediators Inflamm., Wiley 7, 289–294
13 Qin, C., Yang, S., Chu, Y.-H., Zhang, H., Pang, X.-W., Chen, L., et al. (2022) Signaling pathways involved in ischemic stroke: molecular mechanisms and therapeutic interventions. Signal Transduct. Target. Ther., Springer Science and Business Media LLC 7, 215
14 Rehman, S., Nadeem, A., Akram, U., Sarwar, A., Quraishi, A., Siddiqui, H., et al. (2024) Molecular mechanisms of ischemic stroke: A review integrating clinical imaging and therapeutic perspectives. Biomedicines, MDPI AG 12, 812
15 Scassellati, C., Galoforo, A. C., Bonvicini, C., Esposito, C. and Ricevuti, G. (2020) Ozone: a natural bioactive molecule with antioxidant property as potential new strategy in aging and in neurodegenerative disorders. Ageing Res. Rev., Elsevier BV 63, 101138
16 Donat, C. K., Scott, G., Gentleman, S. M. and Sastre, M. (2017) Microglial activation in traumatic brain injury. Front. Aging Neurosci., Frontiers Media SA 9, 208
17 Bourne, J. H., Suthya, A. R., Wanrooy, B. J., Wilson, J. L., Wen, S. W., Bastow, C. R., et al. (2025) Microglia are prominent producers of inflammatory cytokines during the hyperacute phase of ischemic stroke. Commun. Biol., Springer Science and Business Media LLC 8, 1193
18 Malik, S., Alnaji, O., Malik, M., Gambale, T., Farrokhyar, F. and Rathbone, M. P. (2023) Inflammatory cytokines associated with mild traumatic brain injury and clinical outcomes: a systematic review and meta-analysis. Front. Neurol. 14, 1123407
19 de Sire, A., Marotta, N., Ferrillo, M., Agostini, F., Sconza, C., Lippi, L., et al. (2022) Oxygen-Ozone Therapy for Reducing Pro-Inflammatory Cytokines Serum Levels in Musculoskeletal and Temporomandibular Disorders: A Comprehensive Review. Int. J. Mol. Sci. 23 https://doi.org/10.3390/ijms23052528
20 Calderon, R. O., Attema, B. and DeVries, G. H. (1995) Lipid composition of neuronal cell bodies and neurites from cultured dorsal root ganglia. J. Neurochem., Wiley 64, 424–429
21 Maes, M., Brinholi, F. F., Michelin, A. P., Matsumoto, A. K., de Oliveira Semeão, L., Almulla, A. F., et al. (2023) In mild and moderate acute ischemic stroke, increased lipid peroxidation and lowered antioxidant defenses are strongly associated with disabilities and final stroke core volume. Antioxidants (Basel), MDPI AG 12, 188
22 Bocci, V. A., Zanardi, I. and Travagli, V. (2011) Ozone acting on human blood yields a hormetic dose-response relationship. J. Transl. Med., Springer Science and Business Media LLC 9, 66
23 Armeli, F., Mengoni, B., Menin, M., Martínez-Sánchez, G., Martinelli, M., Maggiorotti, M., et al. (2025) Ozone saline solution polarizes microglial cells towards an anti-inflammatory phenotype. Molecules, MDPI AG 30, 3932
24 Clavo, B., Catalá, L., Pérez, J. L., Rodríguez, V. and Robaina, F. (2004) Ozone therapy on cerebral blood flow: A preliminary report. Evid. Based. Complement. Alternat. Med., Wiley 1, 315–319
25 Yan, F., Tang, H., Wang, L., Huang, L. and Zhang, J. (2022) Editorial: Mitochondrial dysfunction in stroke. Front. Aging Neurosci., Frontiers Media SA 14, 888952
26 Cheng, G., Kong, R.-H., Zhang, L.-M. and Zhang, J.-N. (2012) Mitochondria in traumatic brain injury and mitochondrial-targeted multipotential therapeutic strategies: Mitochondria in traumatic brain injury. Br. J. Pharmacol., Wiley 167, 699–719
27 Lee, D. H., Kang, D.-W., Ahn, J. S., Choi, C. G., Kim, S. J. and Suh, D. C. (2005) Imaging of the ischemic penumbra in acute stroke. Korean J. Radiol., XMLink 6, 64–74
28 Pucadyil, T. J., Chipuk, J. E., Liu, Y., O’Neill, L. and Chen, Q. (2023) The multifaceted roles of mitochondria. Mol. Cell, Elsevier BV 83, 819–823
29 Khatri, N., Sumadhura, B., Kumar, S., Kaundal, R. K., Sharma, S. and Datusalia, A. K. (2021) The complexity of secondary cascade consequent to Traumatic brain injury: Pathobiology and potential treatments. Curr. Neuropharmacol., Bentham Science Publishers Ltd. 19, 1984–2011
30 Akbudak, I. H., Kucukatay, V., Kilic-Erkek, O., Ozdemir, Y. and Bor-Kucukatay, M. (2019) Investigation of the effects of major ozone autohemotherapy application on erythrocyte deformability and aggregation. Clin. Hemorheol. Microcirc., SAGE Publications 71, 365–372
31 Gan, Y., Tian, X., Yao, H., Huo, F. and Feng, Y. (2024) Ozone improves oxygenation and offers organ protection after autologous blood transfusion in a simulated carbon dioxide pneumoperitoneal environment in a rabbit hemorrhagic shock model. Transfus. Med. Hemother., S. Karger AG 51, 164–174
32 Liu, S., Levine, S. R. and Winn, H. R. (2010) Targeting ischemic penumbra: part I - from pathophysiology to therapeutic strategy. J. Exp. Stroke Transl. Med., OMICS Publishing Group 3, 47–55
33 McMillin, J. B. and Dowhan, W. (2002) Cardiolipin and apoptosis. Biochim. Biophys. Acta, Biochim Biophys Acta 1585, 97–107
34 Alimohammadi, M., Khoshnazar, S. M., Khajehpour, H., Izadi, M., Einollahi, B. and Hushmandi, K. (2025) Effect of ozone therapy on oxidative stress indices in chronic inflammatory diseases: A systematic review and meta-analysis of randomized clinical trials. Adv. Redox Res., Elsevier BV 17, 100143
35 Ghaemi, M. and Kheradmand, D. (2025) The gut-brain axis in traumatic brain Injury: Literature review. J. Clin. Neurosci., Elsevier BV 136, 111258
36 Yang, W., Yuan, Q., Li, Z., Du, Z., Wu, G., Yu, J., et al. (2022) Translocation and dissemination of gut bacteria after severe Traumatic Brain Injury. Microorganisms, MDPI AG 10, 2082
37 Chiu, L. S. and Anderton, R. S. (2023) The role of the microbiota-gut-brain axis in long-term neurodegenerative processes following traumatic brain injury. Eur. J. Neurosci., Wiley 57, 400–418
38 Durgan, D. J., Lee, J., McCullough, L. D. and Bryan, R. M., Jr. (2019) Examining the role of the Microbiota-gut-brain axis in stroke. Stroke, Ovid Technologies (Wolters Kluwer Health) 50, 2270–2277
39 Geng Y., Wang W., Ma Q., Peng L.-Q. and Liang Z.-H. (2010) Ozone therapy combined with sulfasalazine delivered via a colon therapy system for treatment of ulcerative colitis. Nan Fang Yi Ke Da Xue Xue Bao, Nan Fang Yi Ke Da Xue Xue Bao 30, 2683–2685
40 Su, Z., Lin, J., Zeng, X., Li, X., Hou, Q., Wang, Q., et al. (2025) Ozone water enema activates SIRT1-Nrf2/HO-1 pathway to ameliorate gut dysbiosis in mice receiving COVID-19 patient-derived faecal microbiota. J. Med. Microbiol., Microbiology Society 74 https://doi.org/10.1099/jmm.0.002038
41 Hiebert, P. and Werner, S. (2023) Targeting NRF2 to promote epithelial repair. Biochem. Soc. Trans., Portland Press Ltd. 51, 101–111
42 Cheng, H., Lu, R., Du, J., Zhao, X. and Zhuang, Z. (2025) A clinical study on ozone autohemotherapy for the treatment of acute ischemic stroke. Front. Med. (Lausanne), Frontiers 12, 1595568
43 Wang, C., Zhu, Y., Liu, W., Ren, L., Wu, Z. and Chen, J. (2024) Efficacy of ozonated autohemotherapy for improvement of myocardial injury following traumatic brain injury. BMC Anesthesiol., Springer Science and Business Media LLC 24, 324
44 Xu, G., Sun, X., An, J., Sun, F., Zhang, C. and Williams, J. P. (2025) Ozone protects from myocardial ischemia-reperfusion injury via inhibition of the NLRP3 inflammasome. Eur. J. Pharmacol., Elsevier BV 997, 177631
45 Oxygen-ozone therapy in meningoencephalitis and chronic fatigue syndrome. Treatment in the field of competitive sports: case report https://www.pagepressjournals.org/ozone/article/view/8176/8432

.svg)





